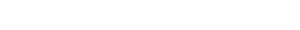A study published in the journal Annals of Clinical and Translational Neurology suggests that most people hospitalized for COVID-19 suffer neurological problems that are symptomatic of their infection. The report states that hospitalized coronavirus patients suffer headaches dizziness and altered brain functions that range from mild to severe.
According to the authors of the study, COVID-19 patients can continue to suffer these neurological problems even after they have recovered from the disease. The researchers from Northwestern Medicine analyzed 509 patients who were hospitalized in the 10 hospitals that make up the network of the health treatment infrastructure. These were people who were admitted into the hospitals between March and April with many of them supported with ventilators.
According to the researchers, 82% of the 509 patients suffered nervous system complications – meaning that 4 out of 5 patients in the study group experienced significant neurologic problems. This fact was established by Dr. Igor Koralnik, a co-author of the study and chief of neuro-infectious diseases and global neurology at Northwestern Medicine.
About 44.8% of the patients complained of muscle pains, and 37.7% reported having headaches. But one-third of the patients suffered more neurological complications such as encephalopathy or altered brain functions. Some of these include loss of memory, confusion, dizziness, loss of taste or smell, multitasking difficulties, and stupor or coma. Koralnik said these difficulties are more likely to be observed in coronavirus patients aged 65 and above.
“This confirms that neurological manifestations are common but often mild,” Dr. Alejandro Rabinstein, a neurologist at the Mayo Clinic. “That is important. Many patients in the hospital with COVID will have muscle aches, will have a loss of smell and taste. Those are reversible and benign.”
The researchers said the neurological complications are caused by the COVID-19 virus and not due to hospitalization because 42% of the patients suffered these complications when they first contracted the disease and were yet to be brought to the hospital.
According to Koralnik, anyone who suddenly loses his ability to smell or taste should suspect coronavirus infection since this appears to be the first sign of the disease. “They should be tested more rapidly and quarantine and trace their contacts to prevent further spread” of the virus,” he added.
The authors of the research further expressed worries that the long-term effects of neurological problems for coronavirus patients are unknown, and that neurologists or neurosurgeons must continue seeing patients even after their discharge from the hospital.
Only nine months into the pandemic,” the authors wrote, “the long‐term effects of Covid‐19 on the nervous system remain uncertain. It is important that people realize the magnitude of these problems. We need to continue to do more research to try to find out why this is happening, especially the brain fog.”
Source: nbcnews.com